
Physician burnout definition
What exactly is physician burnout? In this article, we explore the construct of the burnout syndrome definition as it relates to doctors: a physician burnout definition.

What exactly is physician burnout? In this article, we explore the construct of the burnout syndrome definition as it relates to doctors: a physician burnout definition.

Women physicians still face disproportionate challenges within their medical careers compared to men. Unsurprisingly, those women who face more work-related stressors report less satisfaction with their careers, and more burnout occurs in female doctors.

We are not superheroes. We need to navigate the Fine Line Between Appreciation and Realism.

There is clearly no quick fix to the underlying causes of moral injury in healthcare. This is not a war where a ceasefire can be declared.
So, how do we try to move from the collective moral injury experience of physicians to a systematic change in the structure of medical practice?

“Front-line”, “battle”, “the trenches”. These terms are all too familiar when talking about modern medicine. Why are we referencing war when we should be talking about healing?

We need to talk about physician suicide. Nearly 300 physicians die by suicide every year. National tragedy does not begin to describe it. The agony experienced not just by the victims but their loved ones, colleagues, and patients doesn’t bear thinking about.

What exactly is physician burnout? In this article, we explore the construct of the burnout syndrome definition as it relates to doctors: a physician burnout definition.

Women physicians still face disproportionate challenges within their medical careers compared to men. Unsurprisingly, those women who face more work-related stressors report less satisfaction with their careers, and more burnout occurs in female doctors.
We are not superheroes. We need to navigate the Fine Line Between Appreciation and Realism.

There is clearly no quick fix to the underlying causes of moral injury in healthcare. This is not a war where a ceasefire can be declared.
So, how do we try to move from the collective moral injury experience of physicians to a systematic change in the structure of medical practice?

“Front-line”, “battle”, “the trenches”. These terms are all too familiar when talking about modern medicine. Why are we referencing war when we should be talking about healing?

We need to talk about physician suicide. Nearly 300 physicians die by suicide every year. National tragedy does not begin to describe it. The agony experienced not just by the victims but their loved ones, colleagues, and patients doesn’t bear thinking about.
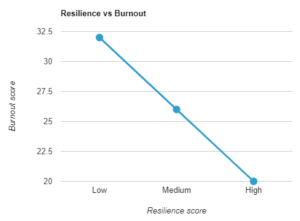
Is there a simple inverse relationship between resilience and burnout? Intuitively, one would think so, but with physicians, it’s never that simple. A recent paper in JAMA Open reveals some startlng findings.

In Part 2, I present the second part of my story: one of physician burnout recovery – how I emerged from the wreckage and rebuilt my life. I sincerely hope that it provides hope for others who are struggling.

If you’ve not heard of Corrigan’s Secret Door, you’re in for a treat. Based on a legendary Irish physician, the Secret Door denotes a metaphorical escape route for busy physicians from their hectic clinics.
My career and life crashed to a halt after 25 years in clinical medicine. I was at one point “suicidal with planning and intent”. Medical knowledge in the hands of a suicidal physician can be deadly. As an affluent, respected physician, confident in my position, well-liked and admired by society, yet suffering inside, why did I not seek help?

Physicians are sick, and it’s getting worse. Yet too few doctors seek help or reach out when we are struggling. Record numbers of us are burning out, becoming mentally ill or addicted, retiring early, and leaving medicine.
In this article, Part 2, I concede that there are some excellent principles differentiating ineffective from effective physician resilience programs. We hope that colleagues and medical leaders designing such programs will find the guidance useful, and further grasp the nettle of addressing the root causes of physician burnout.

Resilience programs, springing up like mushrooms, are a sticking plaster to avoid dealing with the fungating tumor underneath. We have to talk openly about the demands of modern medicine and how these are hurting the healers we need the most.

Practicing medicine is making us physicians sick. Physicians in the US have some of the highest burnout, mental illness, addiction, and suicide rates in the world. Medical student and physician burnout and suicide are a “silent epidemic”.

Modern medicine is no stranger to the toxic trio of burnout, stress, and dissatisfaction, and perfectionism plays the role of the puppet master. It’s time to swap the scalpel for a mirror and reflect. Bowlby’s framework challenges physicians to redefine excellence, shifting from unattainable perfection to a sustainable “good enough” approach.